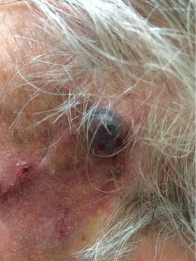
Clinical Image
A Case of Iatrogenic Superficial Temporal Artery Pseudoaneurysm Following Skin Lesion Excision – Key Lessons Learnt
Tan A*, Nizamoglu M and El-Muttardi N
Department of St Andrew’s Plastics and Burns Unit, Chelmsford, UK
*Corresponding author: Alethea Tan, Research Fellow St Andrew’s Plastics and Burns Center, 7 Hazel House, Woodlands Way, M17TH, Chelmsford UK
Published: 18 Jul, 2016
Cite this article as: Tan A, Nizamoglu M, El-Muttardi N. A
Case of Iatrogenic Superficial Temporal Artery Pseudoaneurysm Following Skin Lesion Excision – Key Lessons Learnt. Clin Surg. 2016; 1: 1053.
Clinical Image
We present an interesting case of iatrogenic Superficial Temporal Artery (STA) pseudo aneurysm
following excision of a skin lesion in the left anterior scalp region under local anaesthesia. Given the
large volume of skin lesions in the temple region excised by skin surgeons, we feel sharing this case
will hopefully reinforce the importance of anatomical knowledge and highlight some key lessons to
avoid future occurrences.
An 86 year old gentleman presented with a 1.5cm diameter ulcerated lesion overlying his
left temple region of several years duration. Histology from incision biopsy confirmed ulcerated
nodular Basal Cell Carcinoma. Past medical history consisted of hypertension and he was not on any
anticoagulants. The lesion was excised with a 4mm margin and the resultant defect reconstructed
utilizing a local transposition flap under local anaesthetic. There were no intraoperative complications
and the patient was discharged home. At one week, the flap appeared to be healing well. Five weeks
later, although the wound had healed completely, there was a subcutaneous mass noted at one end
of the scar. The patient reported a small tender lump that appeared approximately two weeks post
operatively that had been gradually enlarging. Initially, this was thought to be an old haematoma.
On further examination the mass was noted to be pulsatile. (Figure 1). The patient was admitted for
emergency surgery within the hour. On secondary exploration, apseudoaneurysm was identified.
This was completely excised and the STA ligated. Subsequent follow up was uneventful.
Recently, Dunbar described 3 cases in which Mohs Micrographic surgery for non-melanoma
cutaneous lesions resulted in pseudoaneurysm; one of the STA, one of the angular artery and one
of the lateral nasal artery [1].
In all the above-mentioned cases, the typical presentation of the
pseudoaneurysm was a painful expansile pulsatile mass between 2 to 4 weeks post intervention. The
treatment of choice was surgical ligation in all cases.
The STA arises from the external carotid artery and courses along the posterior margin of
the condylar process of the mandible. It then crosses the posterior root of the zygomatic process
of the temporal bone [2,3]. Superior to the zygomatic arch, it divides into two large terminal
branches; the frontal branch which lies more anterosuperiorly and the parietal branch which travels
posterosuperiorly [4]. It is important to recognise the course of the
vessel to pre-empt bleeding tendencies intra-operatively and in plastic
surgery, design of flap should incorporate large vessels if possible.
True aneurysms involve all 3 layers of the vessel wall; intima,
media and adventitia as opposed to a pseudoaneurysm which
only involves part of the vessel wall. Given the lack of arterial wall
components in the aneurysmal out-pouching and the presence of
organised haematoma adjacent to the lumen of the STA, a diagnosis
of pseudoaneurysm was made.
It is not uncommon to reveal the STA or its branches during
surgical excision of a cutaneous lesion. At initial surgery, if the STA
was damaged during excision of lesion, the senior author advocates
surgical ligation or transfixion of the damaged vessel rather than
cauterization, no matter how small the tear is. Given the excellent
prognosis, we recommend such cases to be treated acutely. Delay in
treatment not only risks increase in the size of lesion, but also causes
pain and anxiety for the patient. To our knowledge, this is the first case
of pseudoaneurysm of the frontal branch of STA described following
Wide Local Excision (WLE) and local flap reconstruction, highlighting
that this is not a complication limited to Moh’s micrographic
surgical technique. This is an important consideration for plastic and
dermatological surgeons performing WLE procedures regularly.
Figure 1
References
- Dunbar SW, Hurst EA, Pseudoaneurysm formation and repair after Mohs micrographic surgery: a report of 3 cases. JAMA Dermatol. 2014; 150: 546- 549.
- Yonenaga K, Tohnai I, Mitsudo K, Mori Y, Saijo H, Iwai T, et al. Anatomical study of the external carotid artery and its branches for administration of superselective intra-arterial chemotherapy via the superficial temporal artery. Int J Clin Oncol. 2011; 16: 654-659.
- Abul-Hassan HS, von Drasek Ascher G, Acland RD. Surgical anatomy and blood supply of the fascial layers of the temporal region. Plast Reconstr Surg. 1986; 77: 17-28.
- Sinna R, Hajji H, Qassemyar Q, Perignon D, Benhaim T, Havet E, et al. Anatomical background of the perforator flap based on the deep branch of the superficial circumflex iliac artery (SCIP Flap): a cadaveric study. Eplasty, 2010. 10: p. e11.