Case Report
Mosaicoplasty as a Salvage Procedure after Failed Primary Treatment with Silicone Implantation for Focal Osteochondral Lesion of the Knee Joint; a Case Report
Emre TY1*, Atbaşı Z2, Demircioğlu DT3, Seyhan B4 and Uzun M4
1Department of Orthopaedia and Traumatology, Memorial Hizmet Hospital, Turkey
2Department of Orthopaedia and Traumatology, Ankara Military Hospital, Turkey
3Department of Physical Medicine and Rehabilitation, Memorial Hizmet Hospital, Turkey
4Department of Orthopaedia and Traumatology, Etimesgut Military Hospital Ankara, Turkey
*Corresponding author: Tuluhan Yunus Emre, Department of Orthopaedia and Traumatology, Memorial Hizmet Hospital, Halkalı Caddesi Yeşilköy Toplu Konut Sitesi A 31 Yeşilköy, Istanbul, Turkey
Published: 18 Jul, 2016
Cite this article as: SEmre TY, Atbaşı Z, Demircioğlu DT, Seyhan B, Uzun M. Mosaicoplasty as a
Salvage Procedure after Failed Primary Treatment with Silicone Implantation for Focal Osteochondral Lesion of the Knee Joint; a Case Report. Clin Surg. 2016; 1: 1048.
Abstract
The successful treatment of chondral and osteochondral lesions of the weight-bearing surfaces of
the knee joint is a challenge for orthopedic surgeons. If the primary treatment fails, revision or
salvage procedures are even limited particularly when subchondral bone integrity is lost. A 35-yearold
male patient presented with right knee pain, locking and limited range of motion. His past
medical history revealed a femoral osteochondral injury which had been treated with silicone
implantation. The implant was removed, and remaining large osteochondral (5cm2) lesion was
treated with mosaicplasty. At the 5-year follow-up, the patient was symptom-free with almost
complete radiographic incorporation of the graft. This case suggests that mosaicplasty is a good
alternative salvage procedure for osteochondral defects of the femoral condyle even when the
subchondral bone integrity is lost.
Keywords: Mosaicplasty; Cartilage repair; Revision; Silicone implant
Introduction
Focal chondral lesions are a common condition of the knee joint that leads to pain, effusion, locking, and stiffness at initial stages and eventually leads to osteoarthritis and loss of knee function [1,2]. Treatment of these lesions in young patients is particularly important because progression of osteoarthritis may develop quickly at an early age if left untreated. However, mature hyaline cartilage has poor regenerative potential, even in young patients, because it is devoid of vascular, nervous and lymphatic networks [3]. Currently, a wide variety of treatment options exist for focal cartilage lesions of the knee joint ranging from simple chondral abrasion and micro fracture to complex cellbased therapies. Although the decision making is usually based on the patient’s activity level, age, size, extent of chondral defect, and the presence of accompanying problems such as instability and malalingment, there is no comprehensive algorithm on the management and indications of several techniques overlap [4,5]. But, in general micro fracture technique is used as a first line option for small and medium sized defects (less than 2-3cm2). If the primary treatment method fails, there are very limited numbers of techniques that can be used as a salvage procedure particularly when the subchondral bone integrity is lost. Mosaicplasty is a well-defined technique which involves obtaining small-sized cylindrical osteochondral grafts from the minimal weight bearing periphery of the femoral condyles at the level of the patella-femoral joint and transplanting them to prepared defect sites on the cartilage defects. This technique is first described by Hangody et al. [6,7] and presented as a first line treatment modality for cartilage defects weight bearing surfaces of knee joint. Since then, several studies reported good and excellent results of this technique in focal cartilage lesions of the knee joint [8-10]. However, there are few reports regarding its use as a salvage procedure in case of failure of primary treatment especially with large osteochondral defects. Herein, we described a patient who underwent mosaicplasty as a salvage procedure after failed treatment of a large focal osteochondral lesion with a silicone rubber implant (spacer).
Case Report
A 35-year-old male patient employed as an army officer was admitted to our outpatient clinic
with the complaints of right knee pain. The patient was involved in
amateur sports three times a week and had a history of knee pain due
to a traumatic femoral osteochondral lesion which had been treated
with silicone implantation one year ago. The patient's complaints
were alleviated after the surgery but six months after implantation,
pain and loss of function recurred despite conservative treatment
efforts. The patient was evaluated with clinical examination and
radio diagnostic studies. On clinical examination, the patient had an
antalgic gait and the knee range of motion was restricted and painful.
No effusion was detected on the knee joint. Lachman and pivot shift
tests and McMurray sign were negative. The x-ray studies displayed
an osteo-chondral defect in the medial femoral condyle accompanied
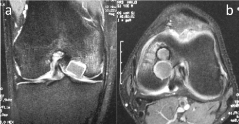
by minimally degenerative changes. MR imaging revealed a silicone
implant in the knee joint as shown in (Figure 1).
Diagnostic arthroscopy was scheduled for exploring the lesion and
the accompanying knee pathologies. During arthroscopic evaluation,
a cartilage lesion at medial femoral condyle and a loosened silicone
implant was observed. We decided to remove the silicone implant
and a medial parapatellar approach was used to expose the silicone
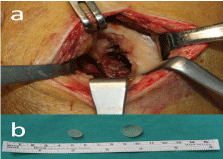
implant. After the removal the lesion size was 5 cm² and 1.5 cm in
depth (Figure 2). Five plugs of osteochondral auto graft 10 x 25 mm in
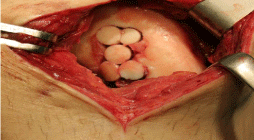
size were harvested from the ipsilateral knee. Standard mosaicplasty
was applied to the defect of the medial femoral condyle as described
by Hangody et al. but the grafts were 1.5cm in length [7] (Figure
3). On postoperative day 1, the patient was mobilized and walked
with crutches. For the following 12 weeks, semi weight-bearing was
permitted on the right extremity, followed by full weight bearing.
The patient was clinically evaluated with Lysholm knee scores before
treatment and during each follow-up. The Lysholm knee score was 55
points preoperatively and increased to 84 points at sixth month and
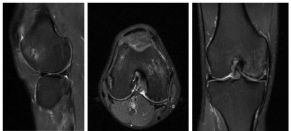
to 92 points at the 5th year follow-up visits. The MRI images of the
patient at 5th year follow-up are shown in (Figure 4). At the 5th year
follow-up, the patient’s mechanical symptoms of the affected knee
have resolved completely along with the pain and his knee no longer
interfered with the functional, social or professional life of the patient
and he was able to perform his sportive activities without a problem.
Figure 1
Figure 1
MRI image of osteochondral lesion in the femoral condyle which had
been previously treated with a silicone implant. Note the fluid accumulation
deep around the implant.
Figure 2
Figure 2
Osteochondral lesion (a) seen on the patella through a knee
arthrotomy after the removal of implants (b).
Figure 3
Figure 4
Discussion
Since silicone rubber has been introduced as a biomaterial, it has
found widespread applications in various fields of medicine such
as catheters, breast implants and small joint arthroplasty. However,
silicone rubber implants may cause several side-effects including
sinovitis and lymphadenopathy [11,12]. There are few reports
regarding its use as a spacer in cartilage defects. Wang and Yu used
hard silicone implants in 20 patients and with cartilage defects and
reported that this implant may delay the pathogenetic progression of
osteoarthritis [13]. During implantation of this implant a socket has
to be prepared which disrupts the subchondral bone. In our case, it
was obvious that the subchondral bone integrity was lost, based on
the observations both during the MRI examination and the surgery.
When there is large osteochondral cartilage defect of the knee
joint in a young patient similar to our case, there are few options for
the treatment. First, fresh frozen osteochondral allografts can be used.
However, this technique has some disadvantages such as high-cost,
risk of viral disease transmission, difficulty in finding matching fresh
donors, allograft failure and high re-operation rate. Gracitelli et al.
[14] reported 41.7% reoperation rate in 163 patients who underwent
Osteo Chondral Allograft (OCA) transplantation as a salvage procedure
after various cartilage repair surgeries. Furthermore, viability of
chondrocytes in such mega osteochondral allografts has been
debated by some authors [15]. Second option can be the use of
osteochondral biphasic scaffolds. A biphasic osteochondral scaffold
unit has two layers. Superficial layer resembles the cartilage tissue
and the deep layer simulates the bone structure. Thus this type of
scaffolds may repair both the cartilage and the bone simultaneously
[16]. Although, in previous studies promising results has been
reported, poor osteochondrogenesis has been show in current studies
[17,18]. As a third option, autologous mosaicplasty can be used in
our case. However, this technique is limited with the availability of
donor osteochondral plugs particularly when the cartilage defect
exceeds 4cm2. In his original article Hangody et al. advised to use
this technique in cartilage defects up to 4cm2 [6,7]. In our case, the
defect size was 5cm2. The second important issue in this technique is
reconstruction of the surface congruity. When the defect is large, it is
not easy to provide the convexity of the femoral condyle.
Conclusion
We described a patient with a large ostechondral defect after failed primary treatment with a silicone rubber implant. This is the first case in current literature which documents the failure of silicone rubber treatment for articular cartilage repair of the knee joint. Mosaicplasty can still be a good option as a salvage procedure even in large defects exceeding 4cm2 in the knee joint, however a meticulous technique should be followed to reconstruct the surface anatomy. Mosaicplasty can reconstruct both bone and the cartilage effectively during the salvage procedure.
References
- Curl WW, Krome J, Gordon ES, Rushing J, Smith BP, Poehling GG. Cartilage injuries: a review of 31,516 knee arthroscopies. Arthroscopy. 1997; 13: 456-460.
- Widuchowski W, Widuchowski J, Trzaska T. Articular cartilage defects: study of 25,124 knee arthroscopies. Knee. 2007; 14: 177-182.
- Buckwalter JA, Mankin HJ. Articular cartilage: degeneration and osteoarthritis, repair, regeneration, and transplantation. Instr Course Lect. 1998; 47: 487-504.
- Richter DL, Schenck RC Jr, Wascher DC, Treme G. Knee Articular Cartilage Repair and Restoration Techniques: A Review of the Literature. Sports Health. 2016; 8: 153-160.
- Cucchiarini M, Henrionnet C, Mainard D, Pinzano A. New trends in articular cartilage repair. J Exp Orthop. 2015; 2: 8.
- Hangody L, Kish G, Kárpáti Z, Szerb I, Udvarhelyi I. Arthroscopic autogenous osteochondral mosaicplasty for the treatment of femoral condylar articular defects. A preliminary report. Knee Surg Sports Traumatol Arthrosc. 1997; 5: 262-267
- Hangody L, Ráthonyi GK, Duska Z, Vásárhelyi G, Füles P, Módis L. Autologous osteochondral mosaicplasty. Surgical technique. J Bone Joint Surg Am. 2004; 86-86A: 65-72.
- Hangody L, Dobos J, Baló E, Pánics G, Hangody LR, Berkes I. Clinical experiences with autologous osteochondral mosaicplasty in an athletic population: a 17-year prospective multicenter study. Am J Sports Med. 2010; 38: 1125-1133.
- Emre TY, Ege T, Kose O, Tekdos Demırcıoglu D, Seyhan B, Uzun M. actors affecting the outcome of osteochondral autografting (mosaicplasty) in articular cartilage defects of the knee joint: retrospective analysis of 152 cases. Arch Orthop Trauma Surg. 2013; 133: 531-536.
- Marcacci M, Kon E, Zaffagnini S, Iacono F, Neri MP, Vascellari A, et al. A Multiple osteochondral arthroscopic grafting (mosaicplasty) for cartilage defects of the knee: prospective study results at 2-year follow-up. Arthroscopy. 2005; 21: 462–470.
- Christie AJ, Weinberger KA, Dietrich M. Silicone lymphadenopathy and synovitis. Complications of silicone elastomer finger joint prostheses. JAMA. 1977; 237: 1463-1464.
- Perlman MD, Schor AD, Gold ML. Implant failure with particulate silicone synovitis (detritic synovitis). J Foot Surg. 1990; 29: 584-588.
- Wang M, Yu C. Silicone rubber: an alternative for repair of articular cartilage defects. Knee Surg Sports Traumatol. Arthrosc. 2004; 12: 556-561.
- Gracitelli GC, Meric G, Pulido PA, McCauley JC, Bugbee WD. Osteochondral Allograft Transplantation for Knee Lesions after Failure of Cartilage Repair Surgery. Cartilage. 2015; 6: 98-105.
- De Caro F, Bisicchia S, Amendola A, Ding L. Large fresh osteochondral allografts of the knee: a systematic clinical and basic science review of the literature. Arthroscopy. 2015; 31: 757-765.
- Li X, Ding J, Wang J, Zhuang X, Chen X. Biomimetic biphasic scaffolds for osteochondral defect repair. Regen Biomater. 2015; 2: 221-228.
- Delcogliano M, de Caro F, Scaravella E, Ziveri G, De Biase CF, Marotta D, et al. Use of innovative biomimetic scaffold in the treatment for large osteochondral lesions of the knee. Knee Surg Sports Traumatol Arthrosc. 2014; 22: 1260-1269.
- Christensen BB, Foldager CB, Jensen J, Jensen NC, Lind M. Poor osteochondral repair by a biomimetic collagen scaffold: 1- to 3-year clinical and radiological follow-up. Knee Surg Sports Traumatol Arthrosc. 2016; 24: 2380-2387.