Case Report
Spontaneous Hemoperitoneum Because of a Ruptured GIST without Abdominal Pain
Tateno Y* and Suzuki R
Miyake Central Clinic 937, Kamitsuki, Miyake, Japan
*Corresponding author: Yuki Tateno, Toshima Clinic 105, Toshima, Tokyo, 1000301, Japan
Published: 21 May, 2016
Cite this article as: Tateno Y, Suzuki R. Spontaneous
Hemoperitoneum Because of a
Ruptured GIST without Abdominal Pain.
Clin Surg. 2016; 1: 1004.
Abstract
We experienced a rare case of spontaneous hemoperitoneum because of a ruptured malignant
gastrointestinal stromal tumor (GIST), with only abdominal bloating and no abdominal pain. GIST
is a common mesenchymal tumor of the gastrointestinal tract. Because of the high vascularity of
the tumor, GISTs are frequently associated with gastrointestinal bleeding. Most patients present
with abdominal pain at the onset of rupture, and the absence of abdominal pain complicated the
management of this patient. To confirm or exclude a diagnosis of hemoperitoneum combined with
a gastric submucosal tumor and intra-abdominal fluid, careful observation is required.
Keywords: Gastrointestinal stromal tumor; Rupture; Hemoperitoneu; Emergency laparotomy
Background
A gastrointestinal stromal tumor (GIST) is a common mesenchymal tumor of the gastrointestinal tract [1-3]. GISTs are characterized by the over expression of the tyrosine kinase receptor through mutations of the c-kit or PDGFRA genes [4]. Because of its high vascularity, GISTs are frequently associated with gastrointestinal bleeding; however, spontaneous hemoperitoneum because of a ruptured GIST is relatively rare [5,6]. Previous studies reported that most patients with GISTs present with abdominal pain at the onset of rupture [5-7].
Case Presentation
An 83-year-old Asian male presented to our clinic with increasing abdominal bloating without
pain. The patient was in his usual good health until 5 days ago when he began to experience
unexplained abdominal bloating. He had no past medical history of a serious illness, surgery, or
hospitalization.
The patient was alert, with a temperature of 36.3°C, blood pressure of 112/60 mmHg, regular
pulse of 84 beats/min, and a normal respiration rate. A physical examination revealed pale palpebral
conjunctiva, symmetrical abdominal distention, and a palpable mass in the epigastrium; however,
there was no abdominal tenderness. There was no other specific finding on physical examination.
Routine hematological analysis revealed normocytic normochromic anemia with a hemoglobin
level of 8.9 g/dL, white blood cell count of 6000 cells/μL, and blood platelet count of 185,000/μL.
Blood chemistry tests revealed a mild renal dysfunction with a urea
nitrogen level of 40 mg/dL and creatinine level of 1.3 mg/dL. Other
blood chemistry parameters were all within normal limits.
Abdominal plain computed tomography (CT) was performed,
with no contrast dye because of the renal dysfunction, to evaluate
the palpable abdominal mass and bloating, which revealed a large
heterogeneous gastric submucosal mass, measuring approximately
70 × 80 mm (Figure 1), with a massive amount of intra-abdominal
fluid (Figure 2). Based on the tumor size and imaging pattern, this
mass was diagnosed as a malignant GIST. However, it was difficult
to identify the causative underlying disease because of the massive
amount of intra-abdominal fluid. We suspected that the acute intraabdominal
bleeding was because of a ruptured GIST, although the
absence of acute abdominal pain was contradictory to this diagnosis.
In addition, we considered a differential diagnosis of cancerous ascites
due to a malignant GIST because the patient had not undergone
hematological or imaging testing for quite some time, and it was
unclear whether the intra-abdominal fluid and anemia were acute or
chronic.
At this point, we decided to admit the patient to our clinic for
careful observation until the possibility of acute intra-abdominal
bleeding was completely excluded. Three hours after the initial
examination, a second hematological analysis revealed that the
hemoglobin level decreased to 7.1 mg/dL, suggesting acute intraabdominal
bleeding.
Therefore, we decided to perform emergency laparotomy.
Intraoperative findings showed a total of 1700 mL of blood in the
abdominal cavity and a 70 × 80-mm, extraluminal, pedunculated,
solid tumor that arose from the greater curvature of the gastric body,
with no signs of peritoneal dissemination. The peritoneal cavity
was lavaged with 7000 mL of saline, and the tumor was completely
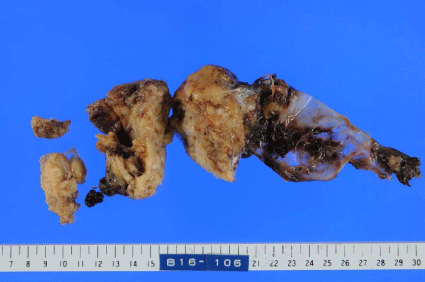
dissected from the stomach. The capsule of the resected tumor had a
puncture (Figure 3) that was sealed with massive blood clots.
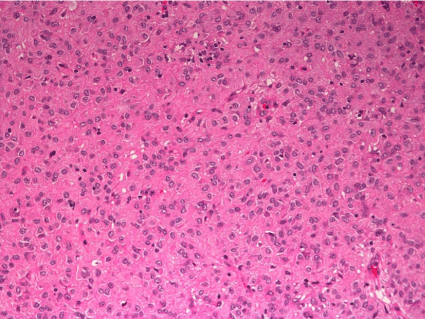
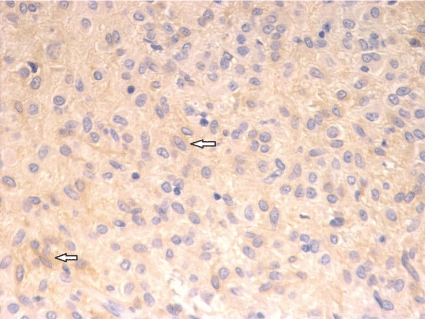
Histological examination revealed spindle cells (Figure 4), and
immunohistological findings were negative for α-smooth muscle
actin, desmin, and S-100 protein but positive for c-kit protein (Figure
5) and CD34.
Based on these findings, the definitive diagnosis was spontaneous
hemoperitoneum because of the rupture of a malignant GIST.
The patient had an uncomplicated postoperative course and was
scheduled for 3 years of adjuvant chemotherapy with imatinib. He
has been followed up for 4 months with no evidence of recurrence.
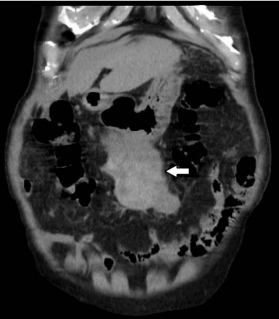
Figure 1
Figure 1
Plain abdominal CT scan revealed a large heterogeneous gastric submucosal mass measuring
approximately 70 × 80 mm (white arrow).
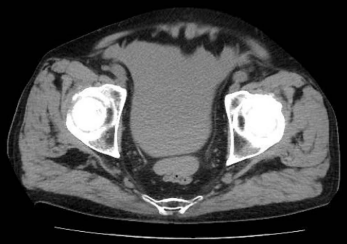
Figure 2
Figure 2
Plain abdominal CT revealed a massive accumulation of intraabdominal
fluid in Douglas’ pouch.
Figure 3
Figure 4
Figure 5
Discussion
We experienced a case of spontaneous non-traumatic
hemoperitoneum without abdominal pain because of a ruptured
GIST. GIST is a common mesenchymal tumor of the gastrointestinal
tract and is most often located in the stomach [1-3]. GISTs are
characterized by the over expression of the tyrosine kinase receptor
through mutations of c-kit or PDGFRA genes and the expression
of the c-kit protein, which is a highly specific marker for the
differentiation of GIST from other mesenchymal tumors [4].
Because of the high vascularity of the tumor, GISTs are frequently
associated with gastrointestinal bleeding. Although several reports
have described spontaneous hemoperitoneum because of the rupture
of GIST, it is a relatively rare condition [5,6]. Most patients present
with abdominal pain at the onset of rupture [5-7]. In contrast, our
patient only presented with abdominal bloating without pain. To
the best of our knowledge, this is a very rare case. However, the
reason why the bleeding was not persistent but rather intermittent
remains unclear. Intraoperative findings revealed that the capsule
of the resected tumor had a puncture that was sealed with a massive
hematoma, suggesting that the intermittent bleeding through the
punctured capsule was the cause of the hemoperitoneum, while
hemostatic properties allowed the clotting blood to seal the puncture.
The absence of abdominal pain made it difficult to arrive at a
differential diagnosis. CT revealed a large gastric mass and a massive
amount of intra-abdominal fluid. The combination of imaging and
clinical findings can mislead physicians to an incorrect diagnosis
such as an advanced gastric tumor with cancerous peritonitis. The
treatment for an advanced gastric tumor with cancerous peritonitis
is commonly chemotherapy or/and palliative care, while emergency
laparotomy is rarely performed [3,8].
Several steps are considered to arrive at a differential diagnosis.
First, the existence of anemia can be helpful in the differential
diagnosis. If a previous hematological study reveals a normal
hemoglobin level that drastically decreases over time, acute intraabdominal
bleeding is strongly suggested [9]. However, one-time
laboratory findings of anemia are insufficient to indicate acute blood
loss because an advanced gastric tumor is often concomitant with
chronic anemia due to gastrointestinal hemorrhage [3,10]. Laboratory
tests were not performed for quite some time in our patient; therefore,
it was unclear whether the anemia was acute or chronic. Second,
previous imaging findings can aid in a differential diagnosis. If recent
imaging findings show a gastric tumor without hemoperitoneum, the
presence of intra-abdominal fluid indicates acute accumulation of the
intra-abdominal fluids such as blood. Imaging exams had never been
performed for this patient; thus, it could not be determined whether
the accumulating intra-abdominal fluid was acute or chronic. Third,
an abdominal tap can be useful. Bloody ascites detected using an
abdominal tap is suggestive of intra-abdominal bleeding. However,
a definitive diagnosis of hemoperitoneum should not solely be based
on using an abdominal tap because cancerous ascites is frequently
bloody [11]. Furthermore, some specific findings of contrastenhanced
CT, such as extravasation and sentinel clot sign, suggest
a diagnosis of tumor-associated hemorrhage [12]. However, such
findings cannot be detected when bleeding is minimal, intermittent,
or has been terminated [12]. In this case, contrast dye could not be
used because of a renal dysfunction; thus, it was not possible to arrive
at a definitive diagnosis of hemoperitoneum based on CT findings.
Although we suspected that the gastric mass was a malignant
gastric submucosal tumor based on CT findings, we could not
determine whether the intra-abdominal fluid was because of chronic
cancerous ascites or acute intra-abdominal bleeding. We carefully
observed the patient and rechecked the hemoglobin level 3 h after
admission, which revealed a decrease in the hemoglobin level,
indicating acute blood loss because of hemoperitoneum. Finally,
emergency laparotomy was performed, and a definitive diagnosis of
spontaneous hemoperitoneum because of a ruptured GIST was made.
The choice for operative or nonoperative management of
hemoperitoneum is dependent on the causative disease or general
condition of the patient [13]. Angiographic embolization is a typical
nonoperative management modality and is often selected for hepatic or
splenic injury [13]. In contrast, the management of hemoperitoneum
because of a ruptured gastric tumor is usually emergency laparotomy
to control bleeding by the resection of the tumor and lavage of the
peritoneal cavity to decrease the dissemination of cancer cells from
the ruptured tumor and to arrive at a definitive pathological diagnosis
[5,7].
Conclusion
We experienced a case of spontaneous hemoperitoneum without abdominal pain because of a ruptured malignant GIST. To confirm or exclude the diagnosis of hemoperitoneum combined with a gastric submucosal tumor and accumulation of intra-abdominal fluid, careful observation is required, and blood tests and imaging examinations should be rechecked to confirm the diagnosis.
Acknowledgment
We would like to express our gratitude to Michio Tanaka for the pathological diagnosis.
References
- Miettinen M, Lasota J. Gastrointestinal stromal tumors--definition, clinical, histological, immunohistochemical, and molecular genetic features and differential diagnosis. Virchows Arch. 2001; 438: 1-12.
- Fletcher CD, Berman JJ, Corless C, Gorstein F, Lasota J, Longley BJ, et al. Diagnosis of gastrointestinal stromal tumors: A consensus approach. Hum Pathol. 2002; 33: 459-465.
- Joensuu H, Fletcher C, Dimitrijevic S, Silberman S, Roberts P, Demetri G.. Management of malignant gastrointestinal stromal tumours. Lancet Oncol. 2002; 3: 655-664.
- Bucher P, Villiger P, Egger JF, Buhler LH, Morel P.. Management of gastrointestinal stromal tumors: from diagnosis to treatment. Swiss Med Wkly. 2004; 134: 145-153.
- Hirasaki S, Fujita K, Matsubara M, Kanzaki H, Yamane H, Okuda M, et al. A ruptured large extraluminal ileal gastrointestinal stromal tumor causing hemoperitoneum. World J Gastroenterol. 2008; 14: 2928-2931.
- Bucher P, Poletti P, Myit S, Morel P. Spontaneous rupture of a gastrointestinal stromal tumour associated with life-threatening non traumatic hemoperitoneum. Can J Surg. 2008; 51: E38-E39.
- Shibata K, Hachiya O, Suzuki T. A case of ruptured Gastrointestinal stromal tumor of the stomach with intra abdominal hemorrhage. Bulletin of the Yamagata University. Medical science: Yamagata medical journal. 2015; 33: 23-28.
- Cabalag CS, Chan STF, Kaneko Y, Duong CP. A systematic review and meta-analysis of gastric cancer treatment in patients with positive peritoneal cytology. Gastric cancer. 2015; 18: 11-22.
- Kasotakis G. Spontaneous hemoperitoneum. Surgical Clinics of North America. 2014; 94: 65-69.
- Ajani JA, Bentrem DJ, Besh S, D'Amico TA, Das P, Denlinger C, et al. Gastric cancer, version 2.2013. Journal of the National Comprehensive Cancer Network. 2013; 11: 531-546.
- Becker G, Galandi D, Blum HE. Malignant ascites: systematic review and guideline for treatment. European Journal of Cancer. 2006; 42: 589-597.
- Lubner M, Menias C, Rucker C, Bhalla S, Peterson CM, Wang L, et al. Blood in the belly: CT findings of hemoperitoneum Radiographics. 2007; 27: 109-125.
- Spahn D. R., Bouillon B, Cerny V et al. Management of bleeding and coagulopathy following major trauma: an updated European guideline. Crit Care. 2013; 17: R76.